Coronaviruses
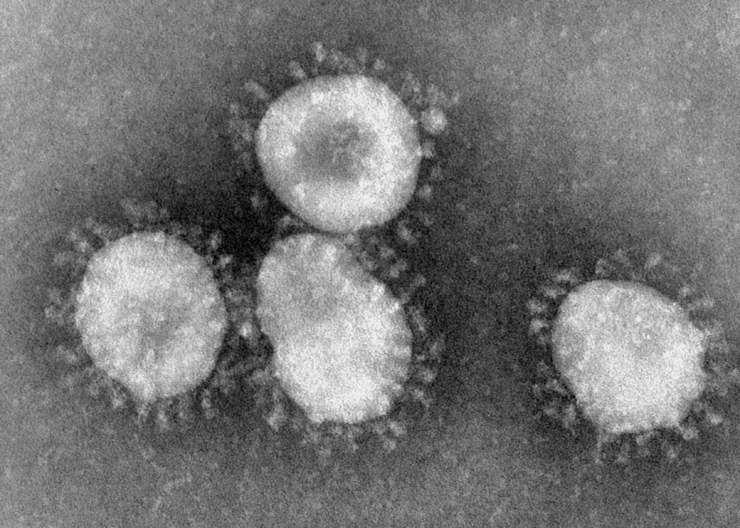
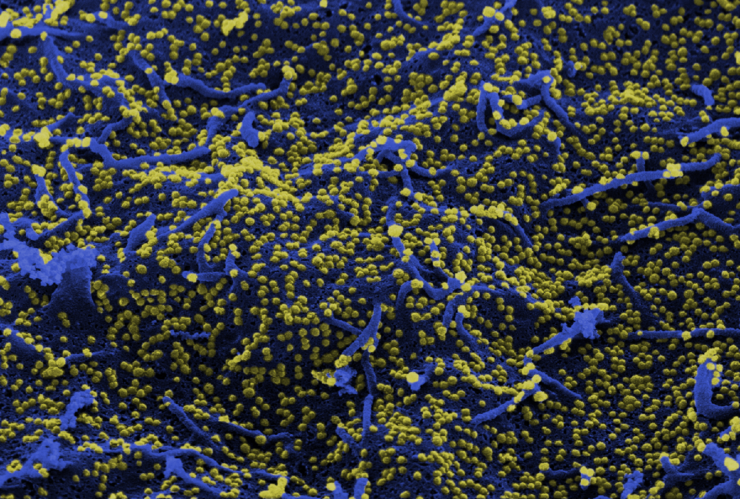
The coronaviruses are a family of viruses that includes a series of very different pathogens. These viruses usually infect mammals, rodents, and birds, but only few coronaviruses adapted to humans. They did this with great success: About one third of all typical "common colds" and some cases of diarrhoea as well are caused by these RNA Viruses, which are the largest of their kind.
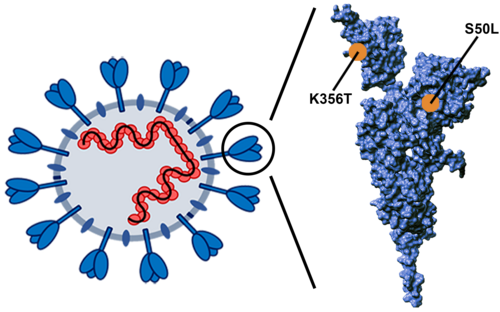
At the end of December 2019, pneumonia occurred in high numbers in the Chinese city of Wuhan. On January 7, 2020, a new type of coronavirus was ultimately identified as the causative agent. This virus is closely related to the SARS virus, which caused a pandemic in 2002, and can be transmitted from person to person. With travel from Wuhan, the new corona virus has also spread to other regions of China and beyond the country's borders to Europe, Australia and the USA. In February 2020, a panel of experts proposed the name SARS-CoV-2 (Severe Acute Respiratory Syndrome Coronavirus-2). The World Health Organization has established the official name COVID-19 (Coronavirus Disease 2019) for the disease caused by SARS-CoV-2.
The virus is transmitted via droplet, aerosol and contact infections. Wearing a mouth-nose-cover reduces droplets and aerosols that may be produced when breathing, speaking or coughing. Thorough hand hygiene with frequent hand washing as well as coughing and sneezing in the crook of the arm not only protects against SARS-CoV-2, but also against infection with other pathogens such as the influenza virus. Social contacts should be reduced to a minimum. Especially in closed rooms, a minimum distance of 1.5 meters to other people is important to reduce the risk of infection. The Robert Koch Institute has compiled detailed information on the novel coronavirus.
We must focus on people who are at particularly high risk of developing severe disease. These people must be given optimum protection and care.

Coronaviruses have been known since the 1960s. Humans had become used to the diseases they elicit until a new coronavirus gained dubious fame: In 2002, the almost 1,000 fatalities caused by the SARS-associated coronavirus (SARS-CoV) showed the world what this species can do.
SARS is an acronym that stands for "severe acute respiratory syndrome", which aptly describes the course of disease. The infection starts out with fever, headache, pain in the neck and muscles, shivers and vertigo and culminates in severe atypical pneumonia with acute shortness of breath and strong coughing. The virus becomes airborne in droplets released by sneezing or coughing and survives for up to 24 hours outside of a host.
SARS - a classic zoonosis?
Where did it come from? One of the explanations implicates masked palm civets, cat-like predators who are indigenous to South and Southeast Asia. They are eaten as food in China, where the SARS pandemic originated. In this case, SARS would be a classical zoonosis, in which a pathogen manages to switch from an animal to a human host. Another possible cause is that a previously known coronavirus that is wide-spread amongst humans mutated to become the aggressive SARS-CoV.
From the time the first patients presented with this dramatic course of disease, it took scientists only 23 days to identify the virus, decipher its genome and develop a diagnostic test, which was done at Bernhard-Nocht-Institute in Hamburg, Germany. The reliable diagnosis, which allowed afflicted persons to be quarantined, made it possible to stop the pandemic. There has been no other case of SARS throughout the world since 2004.
New Cases in the Middle East
Yet another coronavirus is leaving the ranks of mostly harmless pathogens to gain notoriety: In June 2012, patients with severe airway infections and kidney failure were noted in the Near and Middle East. The pathogen is closely related to SARS-CoV and was initially named new coronavirus, or nCoV for short, but has since been renamed MERS-CoV which stands for "Middle East Respiratory Syndrome Coronavirus". According to figures from the World Health Organisation, the virus has infected more than 500 people from 17 countries and killed 145 of those between September 2012 and May 2014.
As indicated by the name of the virus, the focus of the infections is in the Middle East, but this infectious disease is spreading to Europe as well. Cases have been registered in France, Greece, Italy, United Kingdom and Germany - although all of these, without exception, had been acquired in the Middle East.
The origin of this virus is still unknown, but scientists of the Institute for Immunobiology St. Gallen detected extensive similarity to coronaviruses from bats and are presuming that the pathogen may have switched from bats to humans for its host. The recent cases provide reason to conclude that MERS-CoV may have managed not only to switch hosts, but also to spread further in the new host species, i.e. humans. The WHO has issued calls for alertness in all cases involving patients with severe airway diseases.
(jsg)
Involved research groups
-
Pathogen Evolution
 Prof Dr Sébastien Calvignac-Spencer
Prof Dr Sébastien Calvignac-Spencer -
Experimental Virology
 Prof Dr Thomas Pietschmann
Prof Dr Thomas Pietschmann -
Genome Architecture and Evolution of RNA Viruses
 Dr Redmond Smyth
Dr Redmond Smyth -
Biosafety Level 3 Laboratory
 Dr Kai Schulze
Dr Kai Schulze -
Laboratory for Virus-Host Co-Evolution
 Dr Max Kellner
Dr Max Kellner -
Recoding Mechanisms in Infections
 Prof Neva Caliskan
Prof Neva Caliskan -
Laboratory of Transmission Immunology
 Dr Julia Port
Dr Julia Port -
Viral Immunology
 Prof Dr Dr Luka Cicin-Sain
Prof Dr Dr Luka Cicin-Sain