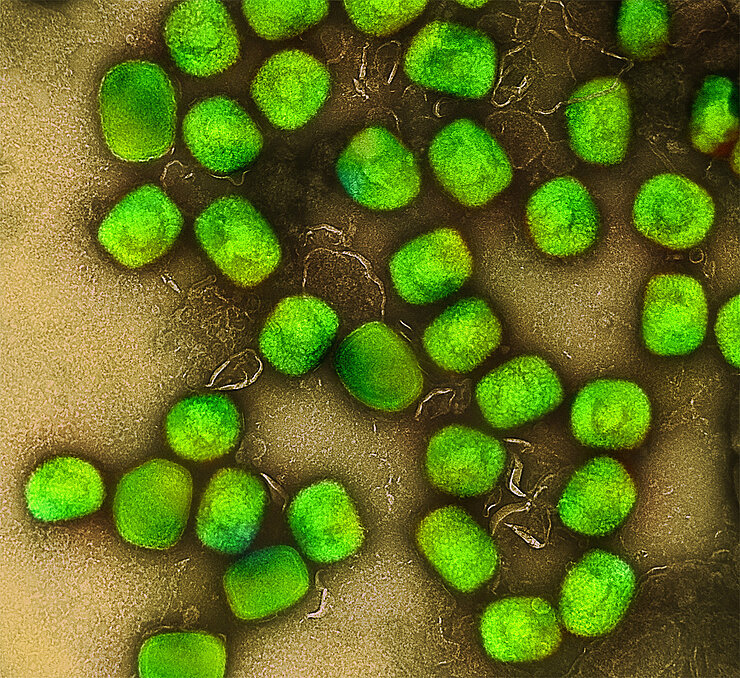
Mpox
A global outbreak brought Mpox to worldwide attention in 2022. The viral disease, which is caused by the monkeypox virus (MPXV), can be transmitted both zoonotically from animals to humans and between humans. The virus is endemic in West and Central Africa, but has now spread globally through various outbreaks. The infection is usually mild. However, it can also be severe or fatal for children, pregnant women, and people with underlying conditions. In addition to general symptoms such as fever, fatigue, and muscle pain, MPXV causes painful skin lesions.
MPXV circulates in two major clades, clade I and clade II – each with subclades a and b – which exhibit distinct differences in virulence, genetic traits, and epidemiology. Clade I was historically associated with more severe disease and higher mortality, while clade II on average causes milder illness. The global outbreak in 2022 was driven by clade IIb, which is marked by fewer systemic symptoms in immunocompetent individuals. This may have facilitated increased human-to-human transmission, but viral adaptation and change in exposure routes are discussed. Clade Ib, the most recent MPXV subclade to emerge, also shows signs of sustained human-to-human transmission. The shift from historically zoonotic, localized transmission to sustained human-to-human spread, primarily also via sexual contact, marks a significant change in MPXV epidemiology.
Animal models for mpox research
Mpox can be transmitted through skin and mucous membrane contact as well as via objects or surfaces. Whether droplet transmission is also possible and whether the susceptibility to infection changes with exposure route has not yet been scientifically clarified. To answer this and other research questions about MPXV transmission, Dr. Julia Port and her research group “Laboratory of Transmission Immunology” at the Helmholtz Centre for Infection Research (HZI) are developing in vitro and animal models for mpox. She has established the multimammate mouse (Mastomys natalensis), a small rodent widespread in large parts of Africa, as an animal model for mpox and has been able to show that the route of transmission is decisive in determining the clinical picture that develops. For example, MPXV Clade IIb causes only mild symptoms in the animal model when administered into the abdominal cavity. In the case of mucosal (rectal or vaginal) exposure, the clinical picture is more pronounced and closer to mpox disease in humans. In addition, infected animals shed more virus. “We need more refined models that replicate the transmission and immunopathological processes we want to study. That may sound trivial, but it's an important prerequisite for us to be able to draw conclusions about humans,” says Port. Using organoids of the skin and the lung, HZI researchers also study mechanisms how MPXV is recognized by the immune system and how the virus evades immune cells. Spatially and structurally similar to actual organs, organoids are miniature models of organs generated from stem cells.
Vaccination protection against mpox
A modified smallpox vaccine is approved in the EU for mpox prevention. It can also be used as post-exposure prophylaxis (PEP) within the first few days after contact with infected individuals. MPXV is related to the now eradicated variola virus, the pathogen that causes smallpox. Due to cross-immunity, smallpox vaccination therefore also provides partial protection against mpox. After the eradication of the smallpox virus, compulsory smallpox vaccination was abolished in 1976 in the Federal Republic of Germany and in 1982 in the former German Democratic Republic. As a result, large population groups no longer have smallpox immunity. Despite its name, the chickenpox virus does not belong to the poxvirus family, but to the herpesvirus family. A chickenpox infection or vaccination therefore does not offer any protection against mpox.
Fire-footed rope squirrels as a mpox reservoir
Members of the poxvirus genus occur in many different mammalian species. However, the individual poxvirus species usually have a narrow host range. While the variola virus has evolved to adapt to humans, MPXV is originally an animal virus. This makes targeted prevention measures difficult, as little is known about which animals the virus circulates in. Researchers at the Helmholtz Institute for One Health (HIOH) achieved a breakthrough when they were able to identify an animal reservoir for the virus. To do this, they investigated an outbreak of mpox among wild sooty mangabeys in Taï National Park in Côte d'Ivoire. Together with the Taï Chimpanzee Project and other partners, they combined ecological, behavioral, and molecular data and were able to show that the virus was transmitted to the primates through the consumption of infected fire-footed rope squirrels. “If we know the animal sources of viruses and the pathways that lead to transmission between species, we can better understand spillover mechanisms. This enables us to develop effective prevention measures that reduce the risk of transmission to humans,” says Prof. Fabian Leendertz, founding director of the HIOH, who has been studying mpox in various mammalian species for many years.
Researchers at the HIOH are working with local partners in the Central African Republic and Côte d'Ivoire to inform the population. They provide information about the risks of infection from contact with certain animal species, such as fire-footed rope squirrels. They also help to establish diagnostics for mpox and other infectious diseases so that outbreaks can be controlled more quickly. The digital tool SORMAS (Surveillance, Outbreak Response Management and Analysis System), developed at the HZI, also contributes to the control of outbreaks. It contains a mpox module and helps to collect data on transmission routes and the geographical distribution of infection cases.
Mpox research at the HZI is not only scientifically significant, but also directly relevant to practice. By developing precise animal models, identifying animal reservoirs, and supporting diagnostic and preventive measures, the HZI is making a decisive contribution to understanding spillover events and preventing or detecting future outbreaks at an early stage. In this way, HZI researchers are translating scientific findings directly into effective measures.
Status: March 2026
(cwe)
Further information
- Information page from the World Health Organization
- HZI podcast InFact with Julia Port: How viruses spread – Mpox, transmission immunology and global health
Involved research groups
-
Pathogen Evolution
 Prof Dr Sébastien Calvignac-Spencer
Prof Dr Sébastien Calvignac-Spencer -
Ecology and Emergence of Zoonotic Diseases
 Prof Dr Fabian Leendertz
Prof Dr Fabian Leendertz -
Laboratory of Transmission Immunology
 Dr Julia Port
Dr Julia Port